Transoral robotic surgery (TORS) represents a cutting-edge advancement in the realm of surgical techniques for addressing tumors and various medical conditions affecting the head and neck. Emphasizing a minimally invasive approach, TORS is performed through the mouth, eliminating the need for external incisions. Utilizing the Da Vinci robotic surgical system, a surgeon adeptly maneuvers robotic arms to operate within the confined spaces of the oral cavity and throat. This article will delve into the intricacies of TORS, evaluating its efficacy, safety, advantages, and the evolving role it plays in modern medicine.
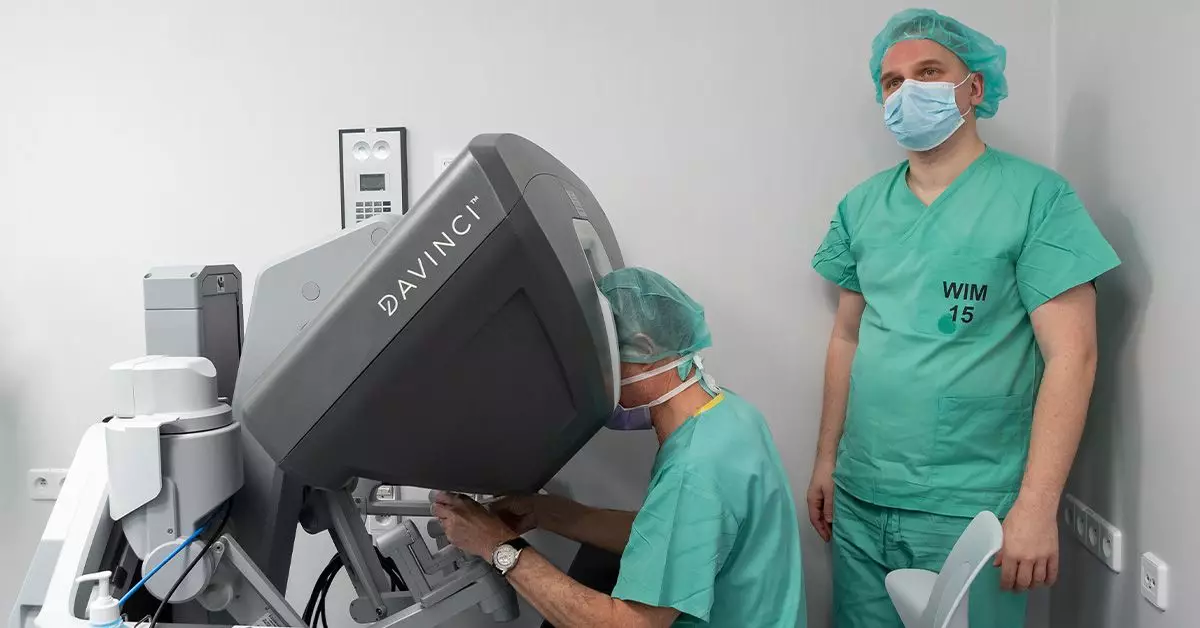
The Da Vinci robotics system comprises three articulated arms, engineered for unique precision. The central arm is embedded with a high-resolution camera that provides the surgeon with a detailed view of the surgical field. In contrast, the two side arms operate like highly dexterous hands, capable of executing complex movements that minimize trauma to surrounding tissues. This sophisticated technology enables surgeons to perform procedures that are traditionally challenging, offering precision that surpasses the capabilities of human hands alone.
Since its FDA approval in 2009 for certain benign tumors and early-stage cancers, the application of TORS has expanded. Recent developments suggest that it is increasingly employed for more complex procedures such as thyroid surgeries and neck dissections. These advancements have prompted further investigations into the safety and effectiveness of TORS across a wider range of head and neck conditions.
Outcomes and Efficacy
Recent research highlights TORS’s positive outcomes compared to nonrobotic surgical methods. A significant study revealed that TORS demonstrates a remarkably low risk of severe complications and excels in achieving complete tumor resection rates. This success not only improves as the surgical team gains experience but also suggests a strong correlation between the number of TORS procedures conducted at a facility and the quality of outcomes.
Moreover, TORS has proven to be an effective diagnostic tool. A recent small-scale study indicated that it can accurately identify primary tumors in head and neck cancer patients, aiding in the formulation of tailored treatment strategies. This dual functionality is an invaluable asset, allowing clinicians to blend diagnostic processes seamlessly with treatment.
As a minimally invasive procedure, TORS boasts numerous advantages over traditional open surgery. Chief among these are shortened hospitalization periods and swifter recovery timelines. Patients often witness less post-operative pain, reduced scarring, and a diminished need for adjunctive treatment methods such as tracheostomy—an incision in the neck for breathing assistance.
Furthermore, a rapid return to normal activities is not uncommon, presenting a significant advantage for patients eager to resume their daily routines. However, it is vital to acknowledge that while robotic surgery bears many benefits, it also introduces risks associated with the technology itself, including potential human error in robot operation and mechanical failures, though these occurrences are infrequent.
Challenges and Considerations
Nevertheless, the journey of TORS is not without its challenges. The risk of complications exists, as evidenced by a reported 10% rate in robotic surgeries. Understanding these risks is crucial for patients weighing their surgical options. Additionally, the physical demands placed on the healthcare team, including potential fatigue due to prolonged robotic control, cannot be overlooked.
Patients can expect to undergo a staging endoscopy prior to TORS to ascertain the tumor’s extent and to evaluate any possible tissue dissemination. General anesthesia is administered, and throughout the procedure, the surgical team closely monitors the patient’s vital signs and comfort levels. Once surgery concludes, recovery typically involves a short stay in the hospital, during which patients may initially rely on temporary feeding tubes. Support from specialists for swallowing and speech can greatly influence post-surgery quality of life.
Post-operative care and long-term monitoring are critical for patients who undergo TORS for head and neck cancers. Regular follow-ups span up to five years to detect any resurgence of cancer, with additional treatments such as chemotherapy or radiation therapy being essential considerations in many cases.
Ultimately, TORS represents a transformative approach to head and neck surgery. While the existing data paints a promising picture, ongoing research is imperative to fully understand the long-term ramifications and to refine techniques further. As robotic surgery continues to evolve, it holds significant potential for enhancing surgical outcomes, reducing patient recovery time, and improving the overall patient experience in a variety of medical contexts.
TORS is establishing itself as a viable and effective technique in the surgical landscape, blending advanced technology with clinical expertise. As healthcare professionals and patients alike embrace this innovative approach, the overall goal remains constant: to achieve optimal health outcomes while minimizing patient discomfort and disruption. Those considering this surgical option should engage closely with their healthcare providers to make informed decisions tailored to their unique circumstances.

Leave a Reply